The hidden root of your gut symptoms
By Chelsea Sanfilippo, MS, RDN
If you’ve read my previous post on reflux, you already know I feel strongly about one thing:
It’s NOT always too much stomach acid causing your symptoms.
Often, it’s not enough.
Now let’s take that conversation one step deeper—because there’s a major player that often gets missed: Helicobacter pylori (H. pylori).
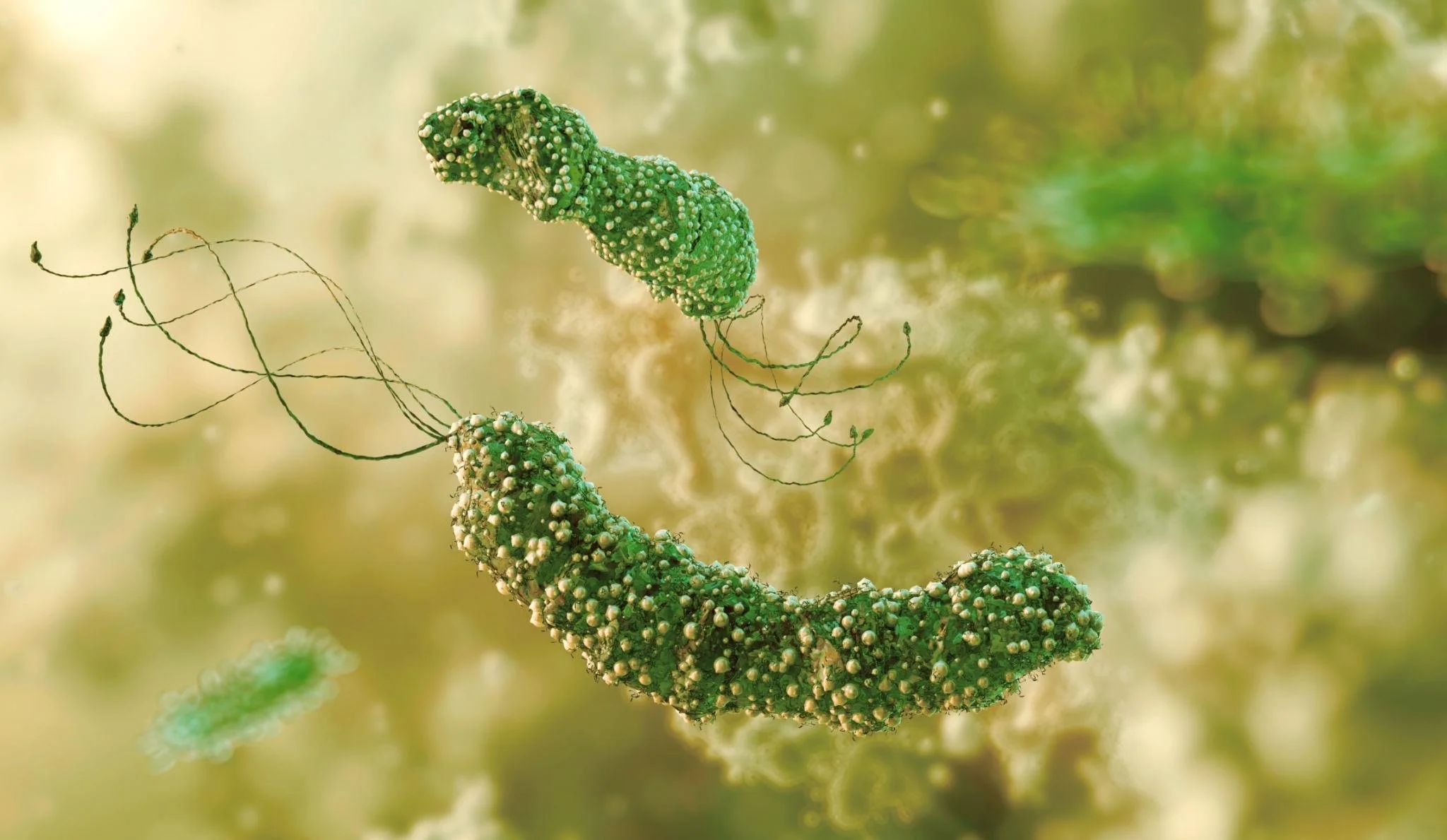
H. pylori is a bacteria that can live in the upper GI tract, primarily the stomach lining. And here’s the interesting part…It’s incredibly good at surviving in a place that’s supposed to be highly acidic. How? It actually reduces stomach acid in its environment to protect itself.
Let that sink in for a second.
H.pylori with flagelly tails containing urease and adhesions on its spiral body.
what does that mean for YOU?
If you have H. pylori, there’s a strong chance you’re not dealing with excess acid…You may actually be dealing with:
LOW stomach acid
Impaired digestion
Increased fermentation (hello, bloating)
A higher risk of reflux and heartburn symptoms
Because of this, the symptoms of low stomach acid can look A LOT like what we’ve been told is “high stomach acid”:
Bloating after meals
Nausea
Burping
That “brick in your stomach” feeling
Reflux or indigestion
While some people remain asymptomatic, many experience symptoms that often get brushed off as “normal”:
Bloating and gas
Nausea (especially on an empty stomach)
Early fullness or loss of appetite
Upper abdominal discomfort or burning
Fatigue
Brain fog
Hair thinning
Increased food sensitivities
Skin issues like rashes or eczema
Why low stomach acid matters (even more with H. pylori)
When stomach acid is low, we lose one of our most important defense mechanisms because stomach acid helps:
Break down protein
Kill off pathogens (including bacteria like H. pylori)
Trigger pancreatic enzyme release & gallbladder contraction
Help absorb critical nutrients like B vitamins, iron & zinc
Reduce antigen exposure
So when H. pylori suppresses stomach acid, it creates a cycle:
Lower acid → easier survival for bacteria
Bacteria thrive → further disrupt digestion
Symptoms persist or worsen
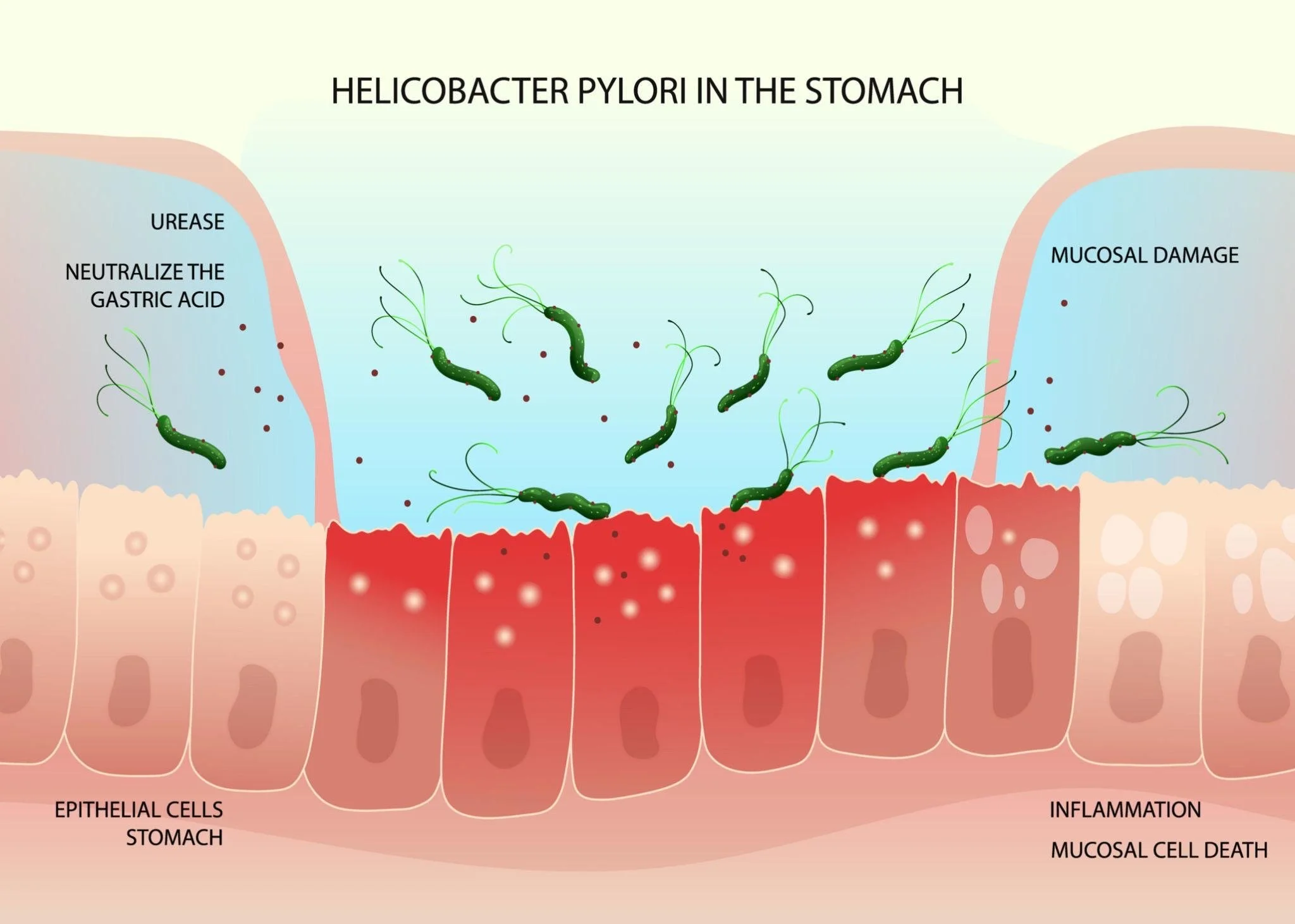
H. pylori can also irritate the stomach lining, contributing to:
Gastritis
Burning or upper abdominal pain
Sensitivity to acidic foods or supplements
This is why jumping into things like apple cider vinegar doesn’t always feel good. Timing and context matter.
So, how does this relate to reflux?
Low stomach acid → food sits longer
Pressure builds
The lower esophageal sphincter (LES) opens
And suddenly…Reflux and heartburn. Again, it’s not always about too much acid—it’s about acid being in the wrong place.
addressing H. pylori is critical
H. pylori is not just sitting quietly in the stomach. When left unaddressed, it may lead to more serious issues like:
Chronic gastritis
Stomach and duodenal ulcers (up to 80%)
Nutrient deficiencies (especially iron & B12)
Long-term digestive dysfunction
Increased risk of stomach cancer
One major reason is its production of urease, which converts into ammonia and neutralizes stomach acid. This allows it to survive, but also weakens your immune defense, increases risk of additional infections and disrupts the entire digestive environment.
While we can’t always avoid it, it’s worth the effort because once it’s present, it can persist for decades if not addressed. Do your best to avoid contaminated food or water and poor sanitation. Good hygiene goes a long way!
H.pylori Can be sneaky!
Though H.pylori is common, affecting ~50% of the global population and ~30–40% in the U.S., it’s very sneaky. It’s not rare, just often missed because it can hide.
Research suggests it may reside within Candida, a type of yeast, which can protect it. This helps explain recurring infections, gut and vaginal yeast patterns and difficulty fully resolving symptoms
It can also shift into a “stealth” form. It has a coccoid form, allowing it to survive harsh environments, evade detection and remain dormant for months; hence why it often gets missed and tests can change over time.
What is the best method of testing for h.pylori?
After working with hundreds of clients, I can confidently say, H. pylori is one of the most common pathogens I find and it is frequently missed in conventional care. This is why it is imperative to choose a good testing method.
Testing options include…
1. Stool Testing (DNA-BASED)
Tests like the GI-MAP provide a deeper look. The GI-Map can tell us about:
H. pylori presence
Virulence factors
Co-infections like Candida - major bonus here given H.pylori hides in Candida
Many other gut health markers
This is where I often see H. pylori show up when other tests have come back “normal.” It allows us to truly look “under the hood” and stop guessing. This is my favorite choice for H.pylori detection.
2. UREA BREATH TEST
Detects active infection in larger amounts.
Non-invasive
Quick
Best for confirming eradication
Does NOT provide virulence factor insight, unfortunately
3. Blood Testing
Shows past exposure, but cannot confirm active infection.
4. Endoscopy
Can detect H. pylori during biopsy, but:
Only samples one area
Can miss infections elsewhere
Accurate, targeted testing matters tremendously because as mentioned previously, H.pylori can hide, shift forms and coexist with other imbalances, which means it can easily be missed without the right approach.
Before Aggressive Protocols, always start with the foundations
Things you can start doing now if you suspect you’re dealing with H.pylori…
Slow down & chew thoroughly
Support your nervous system before meals
Avoid rushed or stressed eating
Be mindful with acidic tools
Trial digestive bitters like Swedish Bitters before meals
Trial small amounts of apple cider vinegar mixed in a glass of water - avoid with gastritis or burning
Take a short walk after meals
→ Supports digestion and motility
Support drainage pathways
→ Liver, gallbladder, and lymphatic flow are key for detoxification and clearing byproducts
Stay well hydrated
→ Supports digestion and elimination
Prioritize nervous system regulation
→ Chronic stress directly impacts stomach acid and gut function
Incorporate gentle movement & deep breathing
→ Supports both digestion and lymphatic flow
Add in the following foods and beverages known to inhibit H.pylori
→ Supports H.pylori inhibition and the general gut environment
Beverages: green tea, cranberry juice, aloe vera
Fruits: berries, pomegranate, apples, grapes
Vegetables: broccoli sprouts, cabbage, garlic, radish
Healthy fats: olive oil, flaxseed oil, fish oil
Fermented foods: yogurt, kefir, kimchi, sauerkraut
Herbs & spices: ginger, turmeric, oregano, thyme
Other: Manuka honey, black cumin seed oil
Emphasize key nutrients:
→ Vitamin C, zinc (especially zinc carnosine), selenium
My Method
I’m all about digging deeper—not guessing.
If you’re experiencing:
Reflux
Bloating
Nausea
Food sensitivities
Ongoing gut symptoms
…it’s time to look beyond surface-level answers. Because when we identify root contributors like H. pylori, we can build a targeted, personalized plan.
Yes, H. pylori is common.
Yes, low stomach acid is common.
Yes, digestive symptoms are common.
But staying stuck without answers? That doesn’t have to be your normal. The goal isn’t to fear H. pylori—it’s to understand when it’s contributing to your symptoms and address it appropriately.
If this resonates with you and you’re ready to explore what’s really going on in your gut…
Email chelsea@guthormonehealth.com to learn more about working together
We can explore whether GI-MAP testing is the right next step for you
You don’t have to keep guessing—there are answers, and there is a path forward.
💛Really hope this blog post helps you in some way! Sending love.
Remember: This post is for informational purposes only and may not be the best fit for you and your personal situation. It shall not be construed as medical advice. The information and education provided here is not intended or implied to supplement or replace professional medical treatment, advice, and/or diagnosis. Always check with your own physician or medical professional before trying or implementing any information read here.